Heat Stress & Athletic Participation Recommended Plan
2025-2026 Recommended Heat Protocols and Procedures for Outdoor UIL Athletic and Marching Band Activities
In 2023, the UIL approved Wet Bulb Globe Temperature (WBGT) as the recommended forecast measurement to be used to monitor environmental conditions during outdoor physical activities. WBGT estimates the effect of temperature, relative humidity, wind speed, and solar radiation using a combination of temperatures from three thermometers.
The American College of Sports Medicine has recommended WBGT guidelines that dictate modifications in activity (work: rest ratios, hydration breaks, equipment worn, length of practice) at given WBGT temperatures to prevent Exertional Heat Stroke. The below table represents modified guidelines from the American College of Sports Medicine regarding:
-
The scheduling of practices at appropriate WBGT levels
-
The ratio of workout time to time allotted for rest and hydration at various WBGT levels
-
The WBGT levels at which activities should be terminated
It is recommended that UIL member schools utilize WBGT to monitor practice and workout conditions and alter practices as outlined in the chart below based on recommendations from the American College of Sports Medicine.
Key Updates to the Heat Plan for the 2025-2026 school year:
- Rapid Cooling Zone Requirement Adjustment
- Everyone is reminded that it is a requirement that all schools have equipment that allows for full body immersion in ice water if an individual is experiencing heat illness and distress. The mandatory rapid cooling zone threshold has been adjusted for the 2025-2026 school year to align with the transition from the green to yellow zones on the WBGT chart.
- WBGT Timing Clarification
- WBGT readings must be taken within 15 minutes prior to the start of practice to ensure accuracy.
- Consistent Monitoring
- When possible, the same individual should take all WBGT readings during the practice window for consistency.
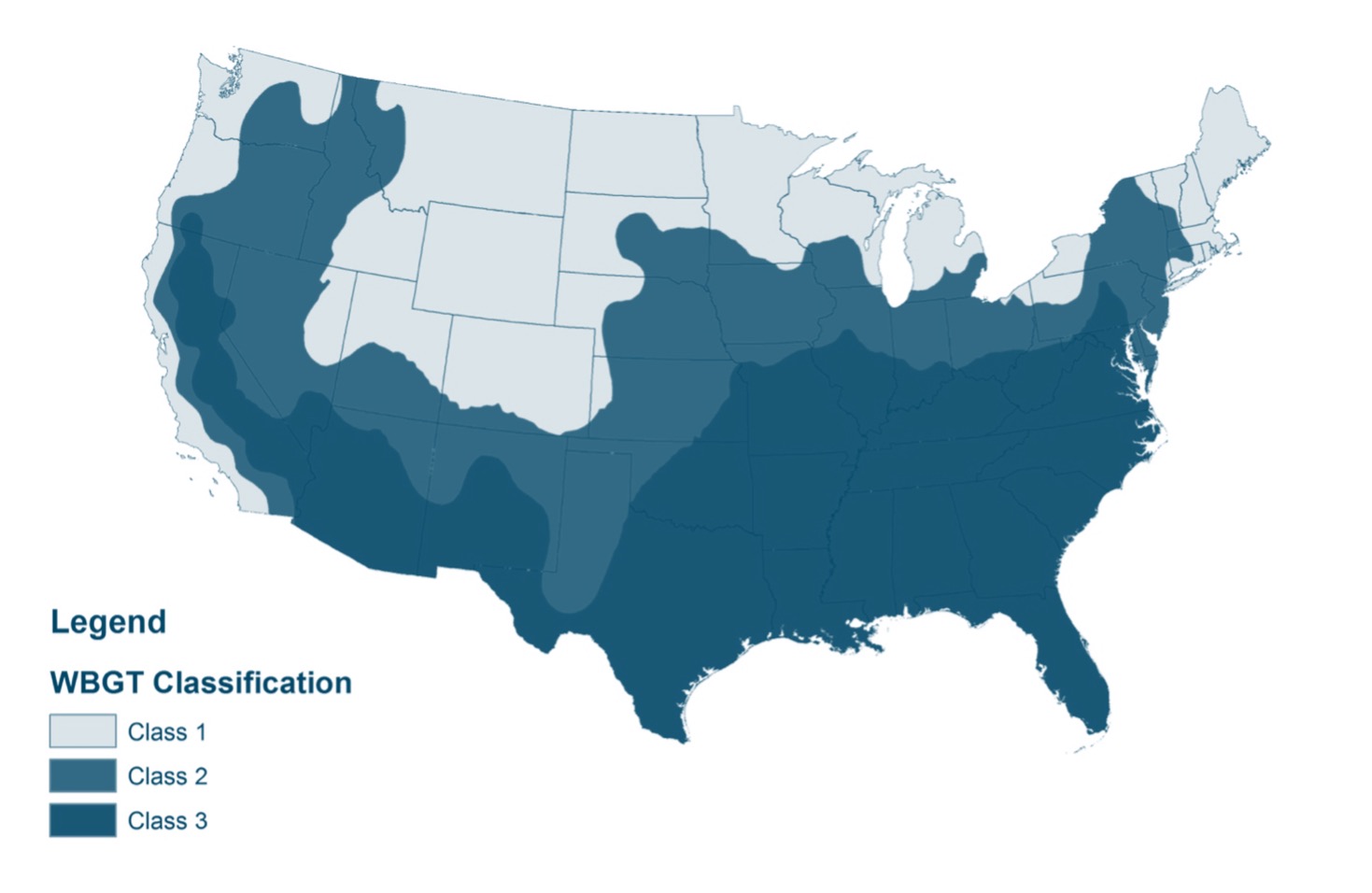

WBGT Forecasting Resource
https://convergence.unc.edu/tools/wbgt/
-
Type your location/address in the white box or select a location on the map.
-
This should be specific to the exact location the practice or contest is located
-
-
Select “Texas UIL Class 2” or “Texas UIL Class 3,” depending on your area, as the flag level guideline
-
Click the “Submit” button at the bottom and scroll down the page to see the forecast.
-
Scroll further down the page to see the WBGT activity guidelines.
WBGT Means and Methods of Measurement when practices are outside in WBGT of 79.7 in Class 2 or 82 in Class 3 or higher
-
It is recommended that schools utilize a scientifically approved instrument that measures Wet Bulb Globe Temperature (WBGT) or other scientifically proven method, such as an internet-based weather station software or application, to monitor the wet bulb globe temperature.
-
If utilizing an on-site instrument, the instrument should be set up 30 minutes prior to practice and should be read 15 minutes prior to the start of practice. If utilizing an internet-based application, the WBGT should also be checked within 15 minutes prior to practice. In both cases, WBGT readings should be taken every 30 minutes during practice.
-
It is recommended that the same person, if possible, take all readings during a practice timeframe.
-
When there’s a change in WBGT from one level to the next, responsible modifications to practice activities should be made based on the above WBGT Activity Guidelines.
-
It is recommended that schools record and keep on file the WBGT temperatures associated for outside practices.
-
Practices are defined as the time period that a participant engages in a coach/director-supervised, school-approved sport or band conditioning-related activity. Practices are timed from when players report to the outside practice/workout area until the players leave the area.
Emergency Action Plans & Procedures for the Prevention of Heat Related Illness
-
Each member school’s emergency action plan must include procedures to address heat emergencies that include onsite rapid cooling using cold-water immersion or equivalent means.
-
Rapid cooling zones must be available for each outdoor athletic and marching band contest, practice, workout, or conditioning session that is held in wet bulb globe temperatures of 79.7 in Class 2 or 82 in Class 3 degrees or higher. Rapid cooling zones are required to have immediate availability of cold-water immersion tubs or tarps that can be filled with ice and water and wrapped around individuals to rapidly cool internal body temperature (TACO method) and are encouraged to include a combination of the following options: ice sponges, towels, water misters, and shade. The presence of an employee or volunteer trained to administer cold-water immersion is recommended.
-
Coaches and directors must adopt a heat injury prevention philosophy by promoting unrestricted access to water at all times and a student- athlete should never be denied access to water.
-
Rest breaks must involve unlimited hydration intake and rest without any activity involved.
Competitions & Possible Modifications to Competitions
-
WBGT practice guidelines and limitations do not apply to UIL competitions, but it is recommended that schools monitor WBGT conditions prior to and during the game and use appropriate emergency action plans for high temperature and humidity. It is advised to consider game time adjustments when experiencing high levels of WBGT readings, in addition to considering use of recommended modifications. Schools may opt to reschedule contests in extreme conditions.
-
Any contest played in WBGT of 79.7 in Class 2 or 82 in Class 3 degrees or higher must have a rapid cooling zone on site and available at all times to allow for full body, rapid cooling of athletes experiencing heat illness.
-
It is recommended that additional appropriate and responsible modifications to contests are made as needed to keep participants safe.
-
Modifications that potentially can be made include (but are not limited to the following):
-
Potentially using additional strategically placed official timeouts (possibly at 6-minute mark or halfway through each quarter) agreed upon by both coaches and officials prior to the start of the game. This would allow the quick stoppage of play and permit officials, athletes, and coaches to quickly hydrate and cool off.
-
Alteration of start times as possible to allow for participation in the best conditions possible
-
Allowing teams that are waiting to warm-up access to air conditioned gyms or locker rooms until organized warm-ups begin.
-
Consider hydration and fueling strategies for participants on long pregame bus rides.
-
Unlimited access to cool water.
-
Shade structures/tents on the sideline to allow for athletes to get out of the direct sunlight.
-
Fans/Misters to allow for evaporative cooling.
-
Ice towels/sponges
-
Lengthening halftimes to allow for more complete cool down and hydration/refueling processes to occur.
-
Having resources that allow athletes to refuel at halftime by providing appropriate snacks
-
A modification, in addition to those listed above, for sub-varsity contests, including middle school, may include reducing the length of quarters if agreed upon by both schools.
-






